Researchers use a quantum Bell test to generate certifiably random numbers, key ingredients for secure network communications.


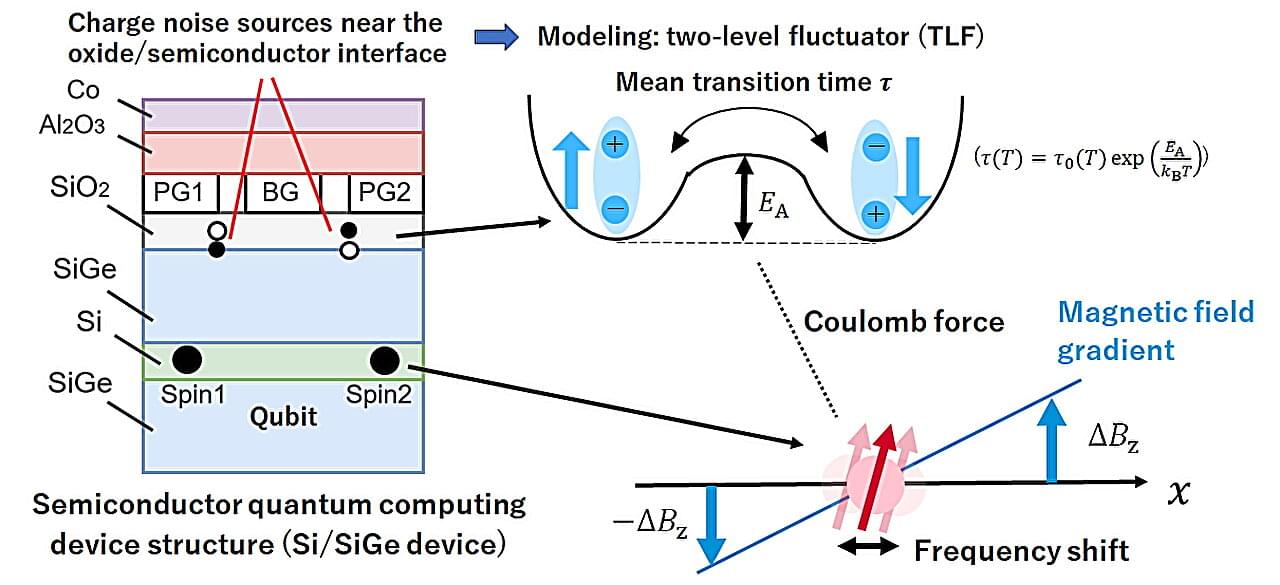
A spin qubit, in which quantum information is encoded in the spin state of an electron, is one of the most promising platforms for quantum computing. Spin qubits exhibit long coherence times and are compatible with advanced semiconductor manufacturing technologies. The leading implementation of spin qubits involves confined electrons inside quantum dots, a nanoscale semiconductor architecture that behaves like a controllable artificial atom. Recent advances have enabled high-fidelity operation of single- and two-qubit gates, exceeding the threshold required for certain surface code quantum error correction techniques.
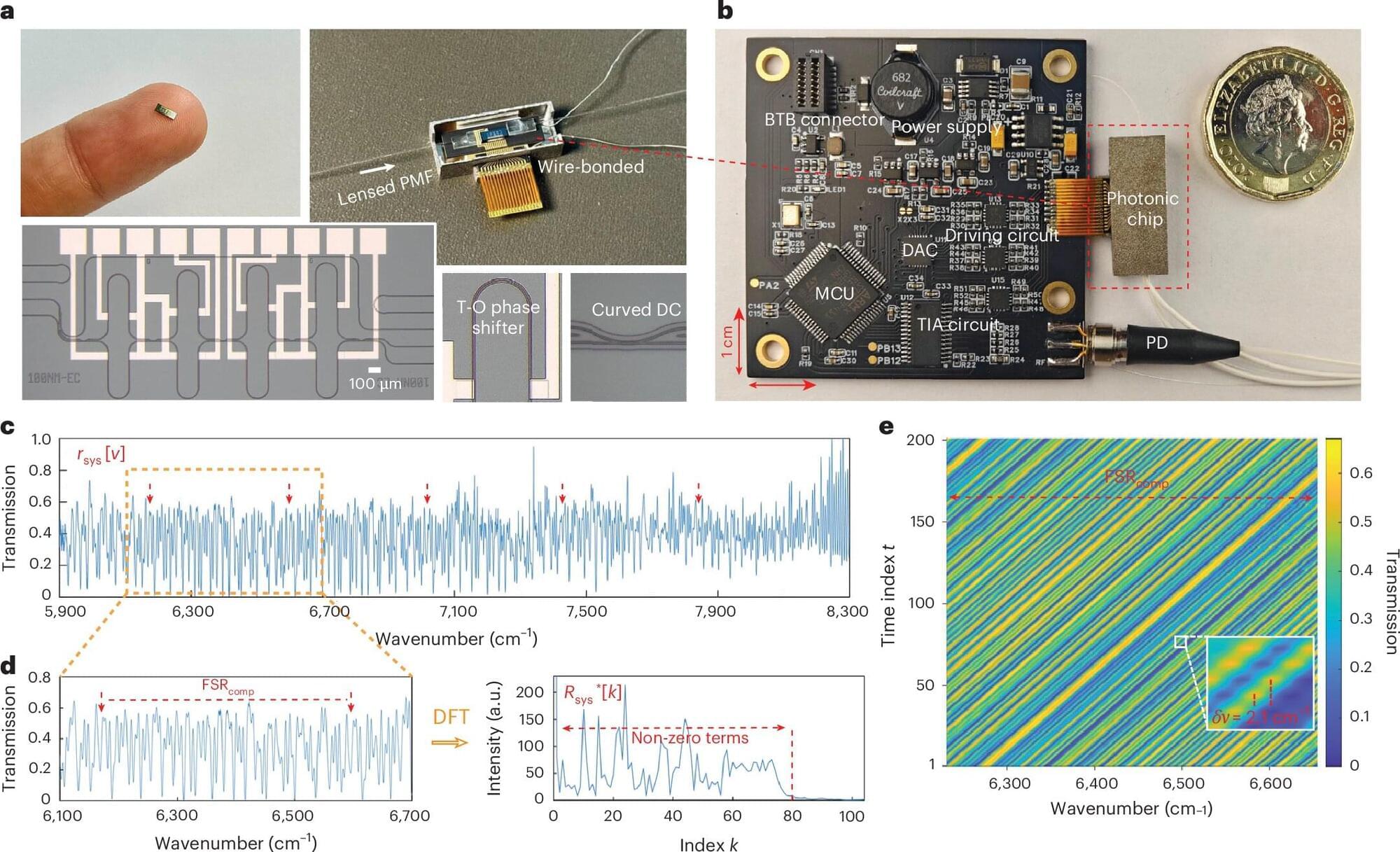
Researchers from the University of Cambridge and GlitterinTech, a startup founded by the same research group, have unveiled a fundamentally new type of optical spectrometer that delivers laboratory-grade precision in a device small enough to be embedded in portable and wearable technologies. By rethinking how spectra are measured and processed, the team has demonstrated a spectrometer costing only around $10, operating at a centimeter scale, and capable of applications ranging from industrial quality control to real-time health care monitoring.
Optical spectrometers underpin countless technologies, from chemical analysis and manufacturing to environmental sensing and medicine. Yet shrinking these instruments has historically involved painful trade-offs: Miniaturized devices typically sacrifice bandwidth, resolution or accuracy, limiting them to rough identification rather than true metrological measurements. The newly reported convolutional spectrometer overcomes these barriers by introducing a conceptually elegant operating principle grounded in the convolution theorem, offering unprecedented performance metrics compared with existing dispersive, Fourier-transform and reconstructive spectrometers.

As artificial intelligence systems grow larger and more powerful, their energy demands are rising dramatically. But recent research from the University of Massachusetts Amherst published in Nature Communications suggests that advanced AI capabilities may be achievable with dramatically lower energy consumption.
A team led by Hava Siegelmann, Provost Professor in the Manning College of Information and Computer Sciences at UMass Amherst, has developed a novel AI that more closely mirrors key aspects of how the human brain operates. Siegelmann and her lab have focused on two complementary goals: enabling AI systems to learn continuously in real time rather than only during a fixed training phase, and dramatically reducing the energy required for intelligent computation.
“Current AI systems are extraordinarily powerful, but they are also extraordinarily energy-hungry,” said Siegelmann. “Our work shows that it is possible to design AI that remains highly capable while operating much more efficiently.”
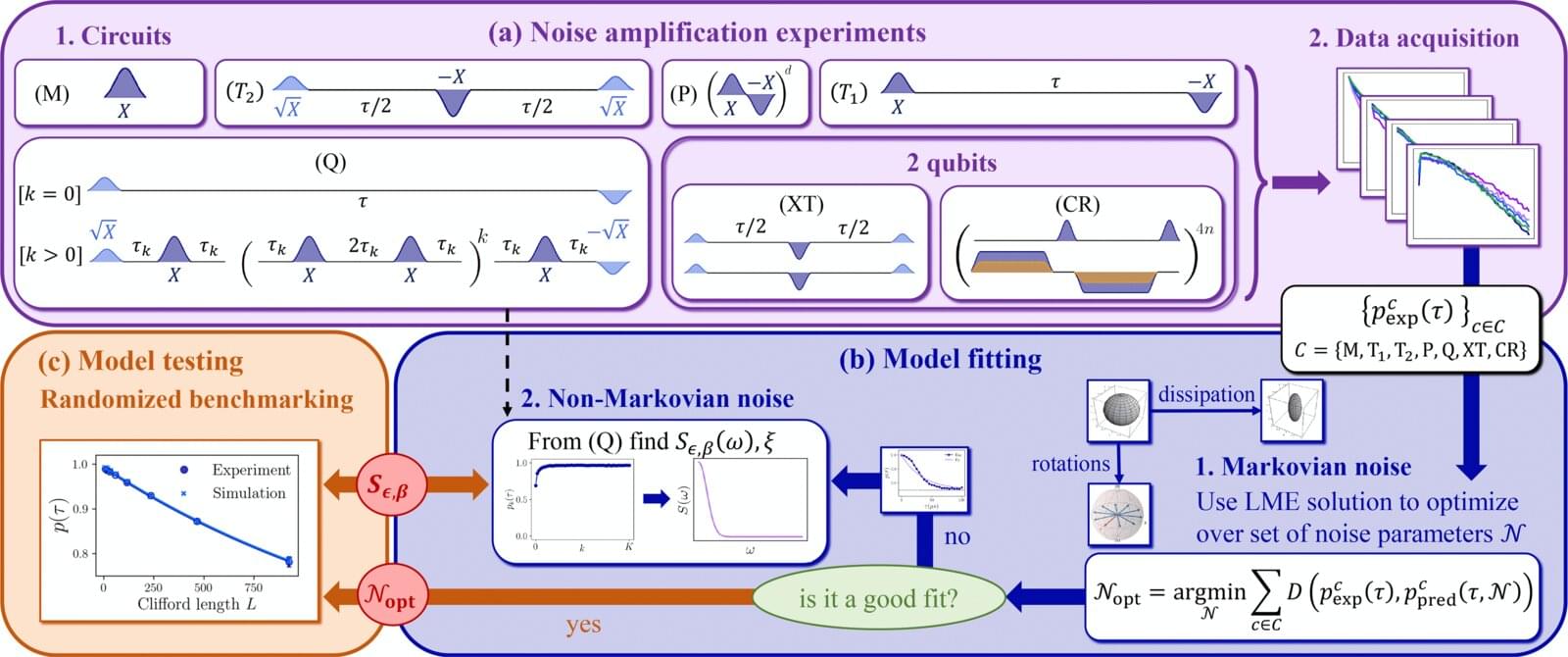
Researchers from the Johns Hopkins Applied Physics Laboratory (APL) in Laurel, Maryland, and Johns Hopkins University in Baltimore have developed a practical, comprehensive noise-modeling framework for a popular class of superconducting quantum processors. Their work, published in the journal PRX Quantum, offers a sevenfold improvement in predictive accuracy over existing approaches.
Quantum bits, or qubits, are intrinsically prone to noise—interference arising from environmental factors such as electrical and magnetic fields or temperature fluctuations—as a result of the extreme sensitivity that makes them so valuable for computing. Developing accurate noise models is key to creating the robust quantum algorithms and resilient error-correction protocols required to build truly fault-tolerant quantum computers.
“To really advance the field, we need models that can predict a wide range of behavior while utilizing a small number of parameters, rather than theoretical models that try to account for all of the fundamental physics at play in quantum interactions,” said project lead Gregory Quiroz, a senior physicist at APL and an associate research professor in the Department of Physics and Astronomy at the Johns Hopkins University Krieger School of Arts and Sciences. “The novelty of our approach lies in a unified and experimentally validated framework that connects multiple noise mechanisms and yields a coherent predictive methodology.”

A new study from the Hebrew University of Jerusalem challenges a long-held assumption in climate science by showing that aerosols—tiny particles suspended in the atmosphere—can either warm or cool the climate, depending on the time scale considered.
Led by Prof. Guy Dagan of the Fredy and Nadine Herrmann Institute of Earth Sciences, the research reveals that aerosol-cloud interactions can produce opposite climate effects in the short and long term. The findings, published in Nature Communications, offer a new explanation for why aerosols remain one of the largest sources of uncertainty in climate projections.
Aerosols come from a variety of natural and human-made sources, including air pollution, wildfires, sea spray and dust. Scientists have long known that these particles influence how clouds form and how much heat Earth retains, but accurately estimating their overall impact on climate has proved difficult.
For over a century, doctors have used electrocardiograms (EKGs) to render the invisible electrical activity of the human heart visible, using the pulse to diagnose disease before it becomes fatal. Now, scientists have invented a way to do the exact same thing for the places where most of humanity lives: cities.
In a recent study published in the Proceedings of the National Academy of Sciences, researchers introduced the concept of the “Urban Pulse.” By using dense, high-frequency satellite imagery, the team successfully tracked the dynamic, real-time metabolic activity of urban environments, effectively measuring the heartbeat of a city.
Zhe Zhu, director of the Global Environmental Remote Sensing (GERS) Laboratory and associate professor of natural resources and the environment in the College of Agriculture, Health and Natural Resources (CAHNR), was the first author. He worked in close collaboration with senior author Karen C. Seto, the Frederick C. Hixon Professor of Geography and Urbanization Science at the Yale School of the Environment, alongside Michail Fragkias of Boise State University and a multi-institutional team of researchers.
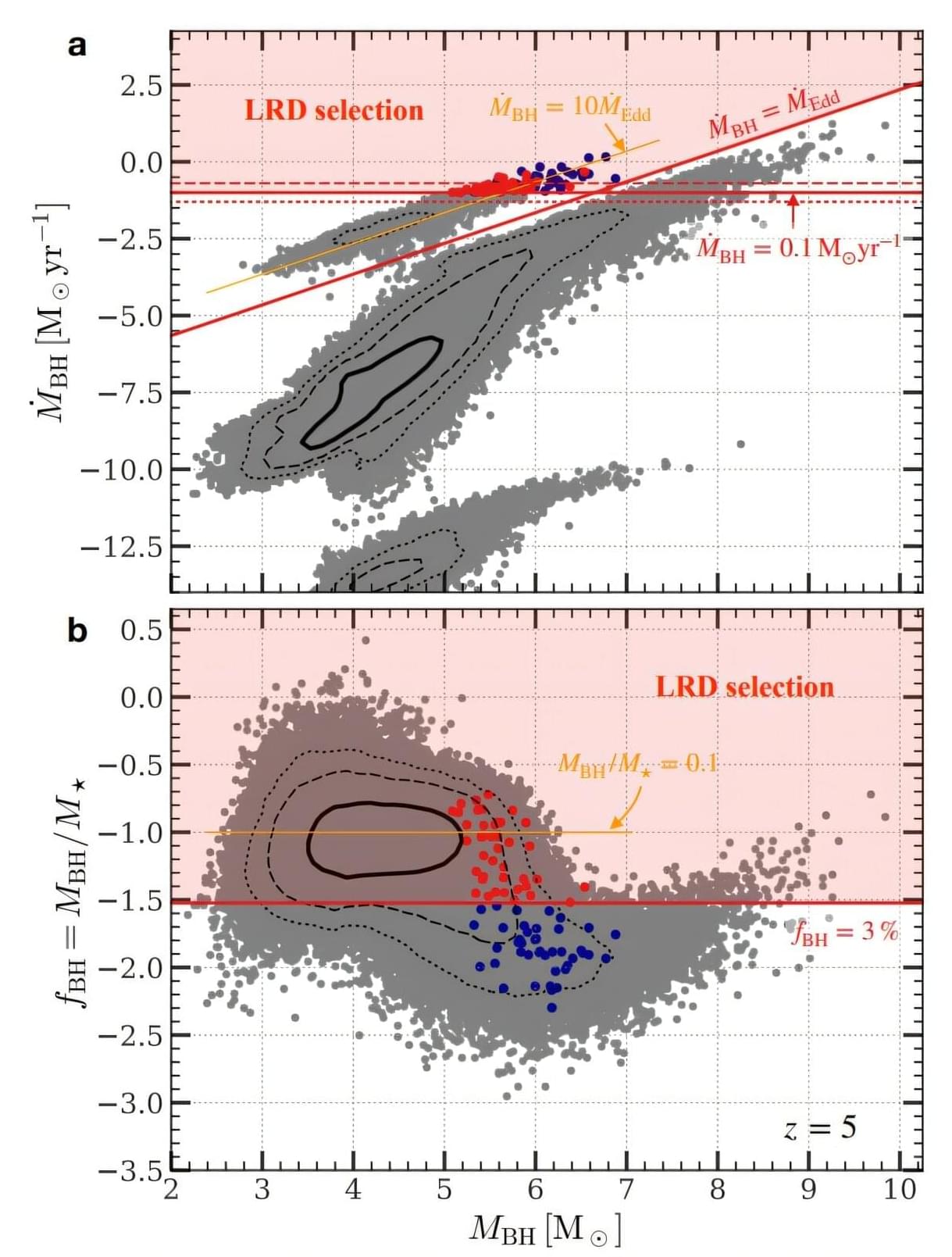
A new theoretical study may have cracked one of the most puzzling discoveries of the James Webb Space Telescope (JWST): Little Red Dots, spotted across the early universe. The paper, posted to the arXiv preprint server on May 29, argues that these objects could be black holes caught in rare, violent bursts of feeding at a rate exceeding theoretical limits.
Since JWST began its survey of the deep universe, astronomers have been puzzled by a class of tiny, faint objects appearing in the early universe in far greater numbers than expected. They have a distinctive V-shaped spectrum—bright in both ultraviolet and optical light, but with a dip in between—along with broad emission lines hinting at active black holes. They also show an absence of X-ray, radio and infrared emission.
They don’t look like ordinary galaxies, and they don’t completely look like quasars, either. What they are has been an open question. Some researchers argue that Little Red Dots may need some outside-the-box physics to explain their origin and nature.
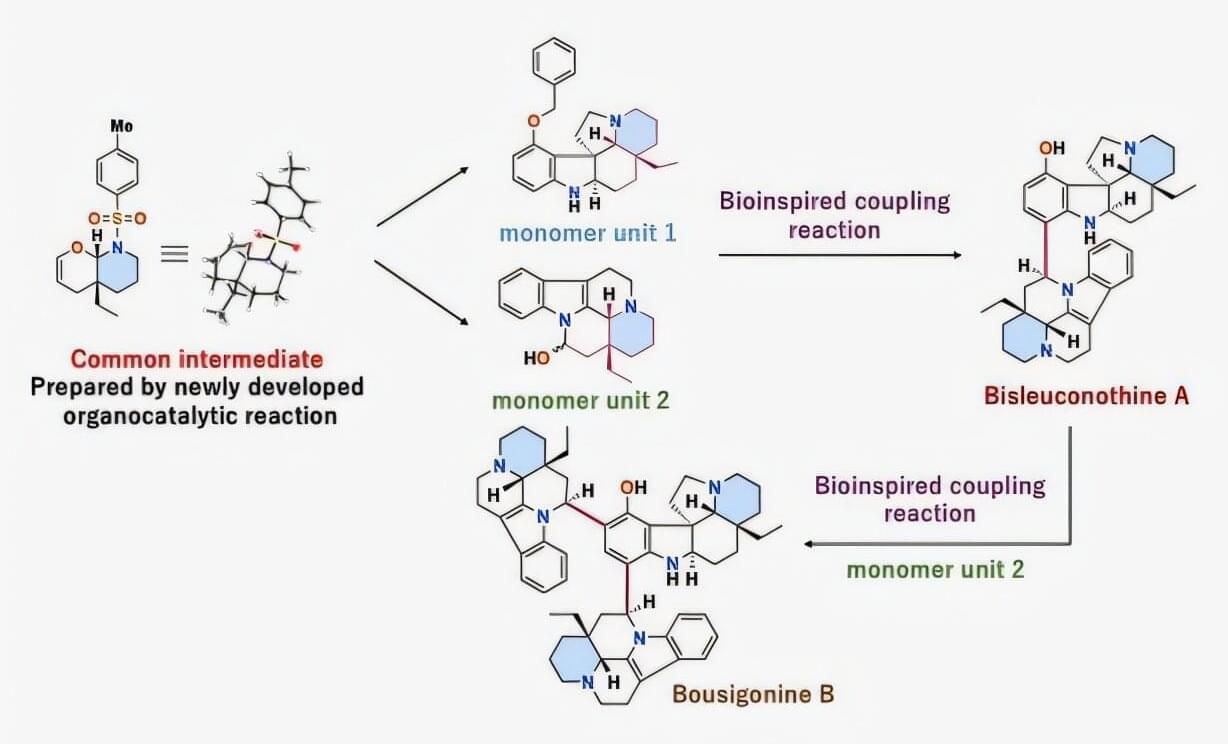
Plants are undeniably one of nature’s most promising sources of new medicines, with monoterpenoid indole alkaloids (MIAs) being a great example. Some intricate compounds are built from multiple-linked chemical units that form highly complex three-dimensional structures. Because of their size and shape, scientists believe such oligomeric MIAs may be able to interfere with specific protein–protein interactions inside cells—a biological target that conventional small-molecule drugs often struggle to reach.
This unusual capability could make MIAs uniquely suited to combat various diseases. Such is the case for bisleuconothine A, an MIA isolated from plant bark in 2010 that has shown strong activity against breast cancer and lung cancer.
Despite their therapeutic potential, these compounds are extremely difficult to produce synthetically in the laboratory. Their structures contain multiple interconnected rings and several precisely arranged stereocenters, meaning their atoms must be assembled in the correct three-dimensional orientation to preserve their biological activity. Because of this, drug development research involving oligomeric MIAs remains limited.

A new study finds that ancient hominins nearly 800,000 years ago deliberately selected specific basalt sources for different stages of tool production rather than simply using whatever stone was available nearby. By tracing the geochemical “fingerprints” of stone tools to both exposed and now-buried basalt flows, the researchers demonstrated that these hominins possessed detailed environmental knowledge, advanced planning abilities, and long-term technological traditions that were maintained and repeated across generations.
A new study published in Scientific Reports provides new insights into the technological behavior and raw material procurement strategies of early Middle Pleistocene hominins at the Acheulian site of Gesher Benot Ya’aqov (GBY). The study uses geochemical analyses of basalt artifacts and nearby basalt sources to trace where the raw material used for tool production came from and to reconstruct how early hominins selected stone within a landscape that has changed dramatically over time. The research was carried out by Dr. Tzahi Golan and Dr. Yoav Ben Dor of the Geological Survey of Israel, and Prof. Naama Goren-Inbar of the Hebrew University of Jerusalem.
GBY, dated to about 780,000 years ago, preserves repeated occupations of Acheulian hominins along the shores of paleo-Lake Hula. Excavations directed by Prof. Goren-Inbar revealed a rich archaeological record, including stone tools made of flint, limestone and basalt, as well as evidence of fire use, plant exploitation, animal processing and fish consumption.