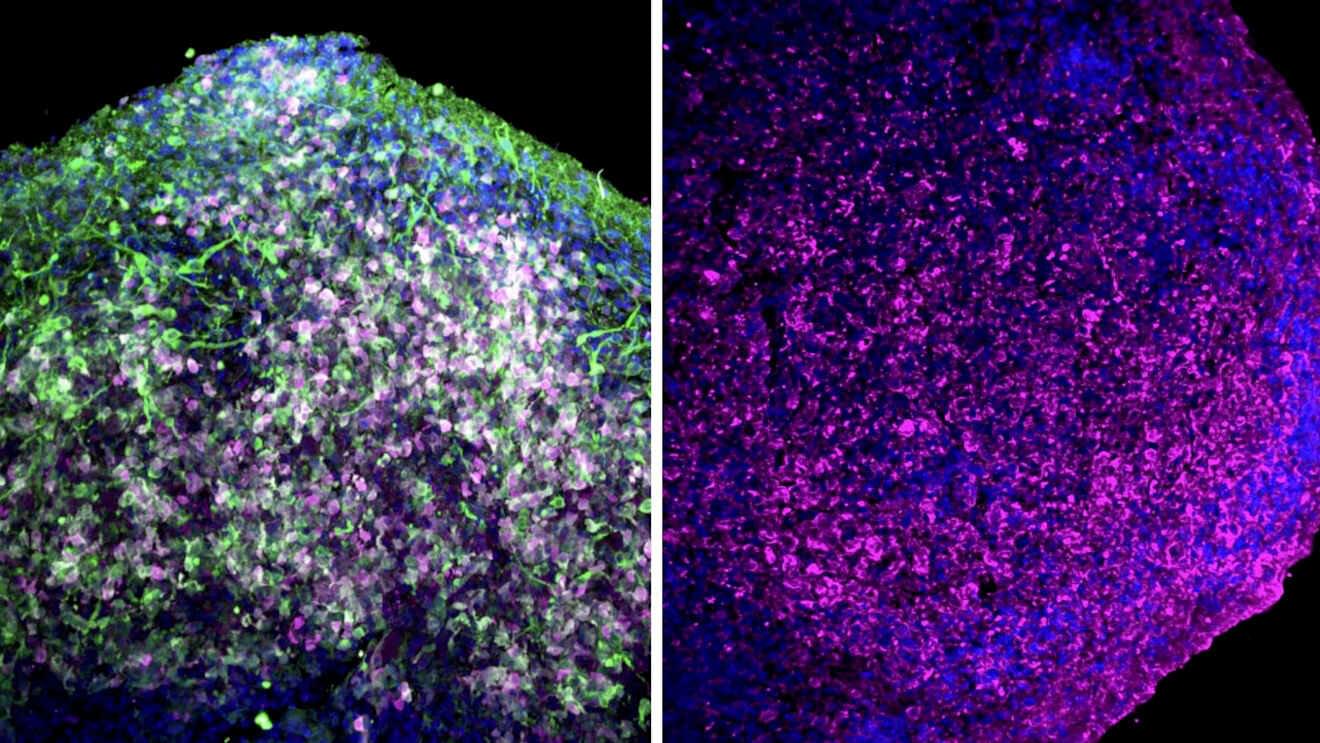
Researchers at the Gladstone Institute have uncovered the molecular mechanism by which APOE4 — the most significant genetic risk factor for Alzheimer’s disease, present in roughly a quarter of the population — begins damaging neural circuits well before any cognitive symptoms emerge. Studying young mice carrying the APOE4 variant, the team found that the gene triggers overproduction of the protein Nell2, which causes neurons to shrink and become hyperactive. Crucially, the degree of early neuronal hyperactivity predicted the severity of memory impairment later in life, even in animals that still showed normal learning and memory at the time of measurement. Strikingly, targeting Nell2 therapeutically was able to reverse these changes even in adult animals, demonstrating that the neurodegeneration is not irreversible and that a window for intervention may exist even after the disease process has begun. The team is currently continuing preclinical testing of this therapeutic strategy.
New findings on the APOE4 gene variant point to a potential therapeutic target for Alzheimer’s disease. From left to right, Gladstone scientists Misha Zilberter, Yadong Huang, and Dennis Tabuena examine findings from their research, which is published in the journal Nature Aging.
For the millions of people who carry the gene APOE4, the strongest known genetic risk factor for Alzheimer’s disease, their brain activity may begin changing long before any memory problems appear. Now, researchers at Gladstone Institutes have uncovered a precise chain of molecular events behind those early changes and identified a potential way to reverse them.
Published in the journal Nature Aging, their new study in mouse models reveals how APOE4 triggers increased production of the protein Nell2, which makes neurons shrink and become hyperactive. The more hyperactive the neurons were in early life, the more severe were the memory problems the mice developed later in life.